Safe healthcare is a team sport. This chapter focuses on the tools and behaviours that help teams communicate clearly and work together effectively.
We'll look at structured tools like SBAR, the importance of safe handovers, and how building trust and psychological safety is the foundation of all great teamwork.
Learning Outcomes
- Describe the four components of the SBAR communication tool.
- Explain the importance of briefings, handovers, and closed-loop communication.
- Define 'psychological safety' and its role in effective teamwork.
Scenario: A Failure to Communicate
Mr Davies, 68, is on a medical ward. His observations are drifting: BP 95/60, heart rate 110. The staff nurse tells the Resident doctor, "Mr Davies doesn’t look right." The doctor is busy and says, "I’ll come later." Two hours later, Mr Davies has a cardiac arrest. The handover was too vague.
Now, let's see what happens when we use a structured tool...
Structured Communication: SBAR
In healthcare, we are not just individuals; we are part of a team. The single most important factor for team success is clear communication. When communication breaks down, safety is at risk.
To prevent this, we can use structured communication tools. The most well-known and effective tool used is SBAR.
SBAR is an "easy to use, structured communication format that enables information to be transferred accurately." It provides a simple framework for any conversation, especially critical ones.
SBAR stands for:
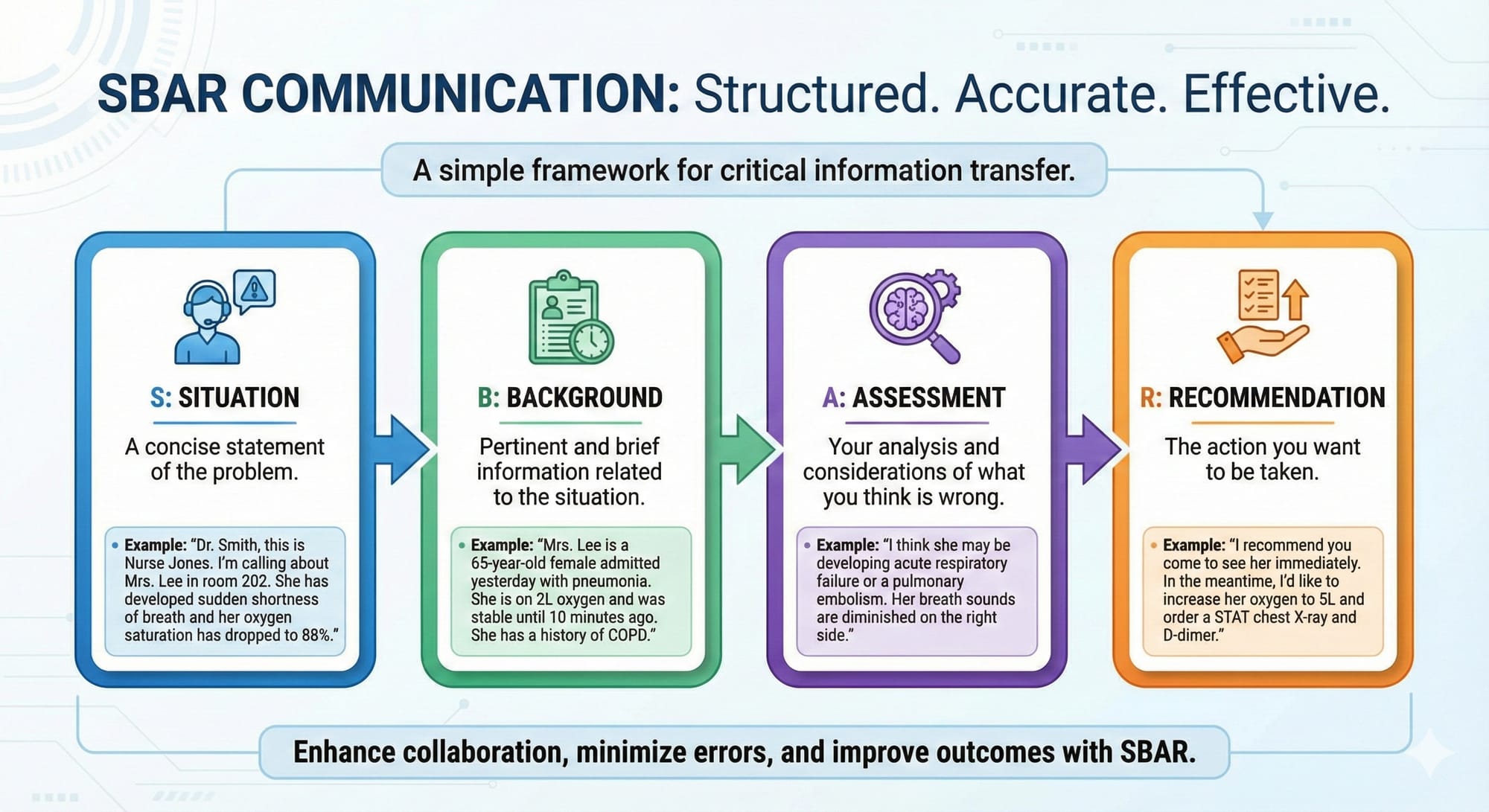
- S = Situation: A concise statement of the problem.
- B = Background: Pertinent and brief information related to the situation.
- A = Assessment: Your analysis and considerations of what you think is wrong.
- R = Recommendation: The action you want to be taken.
📃NHS SBAR Implementation And Training Guide
Handovers, Briefings, and 'Closed Loop'
SBAR is just one part of a wider toolkit for safe team communication.
Clinical Handovers
A handover is one of the highest-risk activities in healthcare. Using a structured process (like SBAR or a standard template) is shown to "reduce communication errors" and ensure critical information is accurately transferred.
Briefings (or 'Huddles')
These are short, proactive team meetings at the start of a shift, a theatre list, or a meeting. A good briefing covers:
- Introductions (especially for new team members).
- An overview of the work (e.g., the theatre list, the ward status).
- Patient-specific concerns (e.g., allergies, complex needs).
- Staffing and resource issues.
Debriefings
These are short meetings at the end of an event (like a shift or a theatre list). They are an opportunity to ask, "What went well? What didn't go well? What can we learn for next time?"
Closed-Loop Communication
This is a simple but vital technique to ensure your message has been heard and understood. The person receiving the information repeats it back to confirm.
Example:
- Doctor: "Please give 10mg of Morphine."
- Nurse: "OK, giving 10mg of Morphine."
This 'readback' 'closes the loop' and prevents errors.
Dr. Roberts (Team Lead)
Resus Room 1 - ActiveSimulation Complete
You have successfully demonstrated Closed Loop Communication.
Remember: Sender gives order → Receiver repeats back → Sender confirms.
The Foundation: Building Trust and Psychological Safety
You can have all the best tools - SBAR, briefings, checklists, but they will not work if the team does not have Psychological Safety.
We defined this in the last module. In a healthcare team, it is the 'shared belief' that you can speak up without fear of negative consequences.
Traditionally, healthcare teams have operated in a "strict hierarchy." A junior nurse may be afraid to challenge a senior consultant, even if they know SBAR and they are sure something is wrong. This is where many safety incidents begin.
Psychological safety is the permission to use the tools. SBAR is the structured way to do it professionally. You need both for a safe team.
Psychological safety allows for "Challenger Safety", where any team member, regardless of seniority, feels safe to say:
- "Can we just pause for a second? I'm not sure this is right."
- "I'm using SBAR because I am concerned about this patient."
The CUS Framework
Sometimes, a polite suggestion isn't heard. In a noisy, high-stress environment, or when facing a steep hierarchy, you need a way to escalate your concerns clearly without being aggressive.
This approach is known as "Graded Assertiveness." CUS provides a universally recognised language to "turn up the volume" on your concern until it is acknowledged. These are not just random words; they are signal words designed to trigger a pause in the team's actions.
C = "I am Concerned"
This is your opening statement. It is a non-threatening way to flag an issue and invite the team to check the situation.
Example: "I am concerned that Mr Davies' blood pressure is drifting lower."
U = "I am Uncomfortable"
If the concern is ignored or dismissed, you move to the next grade. This personalised statement is harder to ignore. It signals that the current plan is causing you specific distress or that your professional boundaries are being crossed.
Example: "I am uncomfortable discharging this patient while his heart rate is still unstable."
S = "This is a Safety Issue"
This is the 'emergency brake.' If the previous steps fail, this phrase stops the line. It shifts the conversation from an opinion to a definitive statement about patient danger.
Example: "Please stop. This is a safety issue. We are about to administer the wrong medication."
For CUS to work, the receiving team member (often the leader) must recognise these keywords. When a junior nurse says, "I am uncomfortable," the leader's role is to pause and ask, "Why? What are you seeing that I am missing?"
Key Takeaways
- Clear communication is critical to patient safety. We use structured tools like SBAR (Situation, Background, Assessment, Recommendation) to transfer information accurately.
- Other key team behaviours include structured handovers, team briefings (huddles), and closed-loop communication (readback).
- Psychological Safety is the foundation of good teamwork. It is the shared belief that it is safe to speak up, ask questions, and admit mistakes.
- Tools like SBAR and a culture of psychological safety are both required. One is the script, the other is the permission to use it.
- When simple communication fails, use CUS for 'graded assertiveness' to escalate your concerns and stop unsafe actions.

